In February 2020, Margaret Downing read an article that terrified her. It predicted that a novel coronavirus spreading around the world would overwhelm U.S. healthcare systems, particularly those in small communities like her town of Yarmouth.
“It was very obvious to me that this was going to be a very bad situation,” Downing, 73, said this month. “There were going to be a lot of people that got sick, a lot of people that died. It required immediate and energetic focus. We needed to get going.”
Downing, who has worked as a lawyer and an affordable housing developer, said small local governments like the one in her town of 8,500 don’t have the capacity or flexibility to respond to an evolving pandemic. So volunteers stepped up.

Yarmouth residents established a task force to educate their community about social distancing, sewed thousands of masks, created a resource website, established a call center at the library, facilitated wastewater testing and helped set up a swab-and-send testing site. A town survey over the summer found 80 percent mask compliance.
Yarmouth’s task force is one of several across the state. Their work may be one reason Maine maintains one of the nation’s lowest COVID-19 infection rates one year after the state’s first case was detected on March 12. Their success could change Maine’s approach to public health even after the pandemic.
Since the virus reached Maine, more than 45,000 cases have been reported statewide, about 1,500 Mainers have been hospitalized and 704 have died as of Friday. Daily case counts, deaths, hospitalizations and the positivity rate all have decreased significantly since the end of 2020. Nearly 19 percent of the population — more than 253,100 Mainers — have received their first vaccine dose.
Early in the pandemic, officials projected that Piscataquis County would be hit hard because it has high rates of poverty and poor health outcomes, according to Sue Mackey Andrews, a task force member in Dover-Foxcroft. The county has one death associated with COVID-19 and maintains one of the lowest case rates.
“I think we surprised them,” Mackey Andrews said. “In some ways we’ve surprised ourselves.”
Many of these local groups helped communicate crucial public health information to communities that statewide offices struggle to reach. Abdulkerim Said, executive director of the New Mainers Public Health Initiative in Lewiston, said COVID-19 has demonstrated how important it is to have people on the ground who look like — and are trusted by — the communities they serve.
“We are local and we speak their language,” he said of his organization’s COVID-19 task force, which primarily works with Somali immigrants and refugees. “(Volunteers) are from their own community, and they are transmitting that information to their community.”
Ten members of five community COVID-19 task forces told The Maine Monitor that their groups posted flyers and updated websites about COVID-19 symptoms, safety protocols, quarantine policies for visitors, testing locations, and most recently where and how to get a vaccine. Some also distributed cleaning supplies, provided food delivery and ride-share services for homebound people, and recruited volunteers for vaccine clinics.
Rebecca Boulos, executive director of the Maine Public Health Association, said the success of these community task forces could alter how the state plans and implements public health initiatives in the future.
“There’s a saying that all politics is local, and I feel that way about public health,” Boulos said. “I’m not suggesting that it replaces state and federal efforts, but having a face to public health in your town is really important because there’s sort of an immediacy of trust.”
The disproportionate impact on Mainers of color
Said, with the New Mainers Public Health Initiative, said he knew from history that pandemics have a disproportionate impact on communities of color and other marginalized groups. When Maine recorded its first COVID-19 case, his organization convened a task force of community leaders from the immigrant community to step up right away instead of waiting for the state or municipal governments to lead.
The task force went door-to-door with community health workers to educate people about why they should get tested for COVID-19. The group also provided hot meals, assisted with employment and housing challenges, trained high school tutors and located a hotel for people to quarantine. This week its members are finalizing videos of interviews with health professionals talking about vaccine hesitancy and why it’s important to get a shot.

Anissa Aden, a community health worker employed with the New Mainers Public Health Initiative, said she went door-to-door with the task force to educate people about the importance of getting tested. Now people call her with questions about the vaccine because they trust her. As someone working within her own community, Aden said she can spend more time explaining the science and answering questions.
“I can talk to them for one or two hours and tell them, ‘You are not alone. We are here with you and we can help you,’ ” Aden said.
Throughout the summer, Maine had the nation’s worst racial disparity for COVID-19 cases, with Black Mainers contracting the virus at a rate 20 times that of white Mainers. Said attributes that disparity to the absence of public health offices in places where the state could have been tracking health outcomes for New Mainers.
Health disparities existed before the pandemic, he said, but COVID-19 revealed gaps in access to healthcare for Mainers of color and the state’s “incompetence” in addressing the health needs of minority groups.
Black Mainers make up 1.4 percent of the population but account for 5 percent of COVID-19 cases, according to the Maine Center for Disease Control and Prevention. White Mainers make up 94 percent of the population but 79 percent of cases. Black Mainers have received 0.7 percent of all first doses.
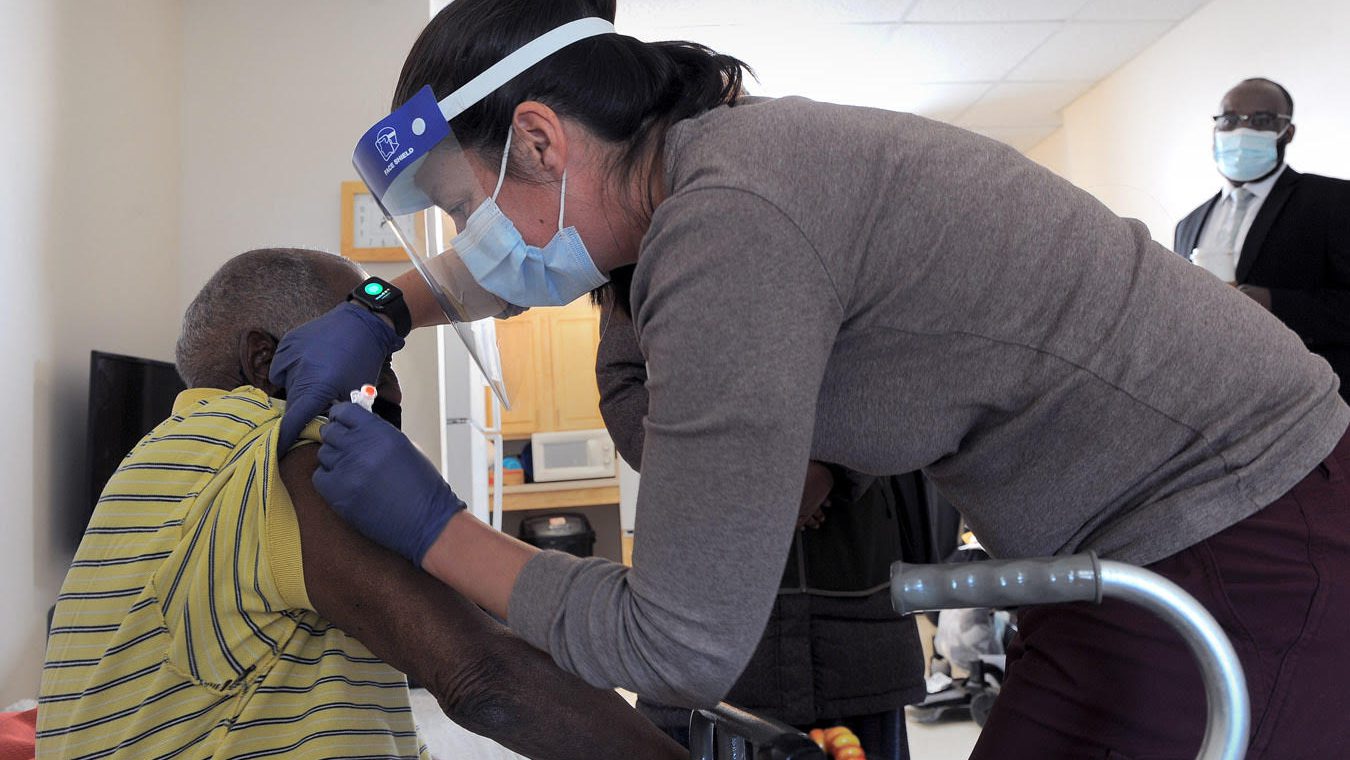
New Mainers have a harder time accessing healthcare, are more likely to have front-line jobs and typically live in larger groups, which makes it difficult to quarantine once exposed to the virus, according to Said.
Dr. Nirav Shah, director of the Maine Center for Disease Control and Prevention, on Thursday said his agency is actively doing outreach in diverse communities to ensure people have “culturally appropriate resources” and help signing up for shots.
“We don’t think those disparities are unavoidable, and we are trying to work deliberately to cut them off and prevent them from happening,” Shah said.
Groups like Said’s are a “vital link” between state efforts and the people working on the ground, Shah said.
“They are able to voice their concerns and give voice to the concerns of their members to make sure that we are hearing them,” he said. “We, in turn, can talk with them about the policies and programs we’re putting into place so that their members and their folks on the ground can take advantage of them.”
To improve the state’s public health system, Said would like to see offices in more major cities so they can collect health data and educate the community. And the state workforce needs to look like the communities they represent, he said.
“The only people that we see are the white people and (they are) telling us from the top to implement their own idea on the plan in our community, which doesn’t work sometimes when the plan comes from the top, not from the grassroots,” he said.
Said envisions the task force helping to bridge this gap as his community continues to deal with the impacts of the pandemic and future health challenges.
‘We definitely kept some people safer’
Sue Mackey Andrews said her task force, which covers Piscataquis County and parts of Somerset and Penobscot counties, focused on making sure people had enough food and fuel. The team includes healthcare professionals, food providers, law enforcement, emergency response and town managers.
There were gaps in healthcare in rural Maine before the pandemic, said Mackey Andrews, who worked in early childhood disability services. She anticipated the pandemic would have a “devastating impact” on her community, which already had high poverty and poor health outcomes.

With unprecedented numbers of people out of work and strains on food providers, demand at food pantries shot up during the pandemic. And advocates worried about people keeping their homes warm throughout the winter.
Emily Poland, a task force member and former school nurse from Dover-Foxcroft, said their group faced considerable resistance to masking and social distancing recommendations. The pandemic was a divisive issue in the community, and county commissioners passed a proclamation challenging the effectiveness of masks and stay-home orders.
When the governor mandated masks in public spaces, there wasn’t a local public health figure who could provide guidance for residents and businesses, Mackey Andrews said. To fight misinformation, the task force brought local leaders together to come up with a uniform message. The group also enlisted local children to make posters about social distancing and masking, and recruited volunteers for the local food shelf and a vaccine clinic conducted by Northern Light Health.
While it’s hard to measure the task force’s success, Poland said masks now are much more common in their community. Mackey Andrews stopped short of saying the task force saved lives, but said, “We definitely have kept some people safer.”
These task forces are “imperative” for the future of public health in Maine, Mackey Andrews said. They allow a more nimble response to a variety of challenges, including the opioid crisis, quality housing, well contamination and teenage suicidal ideation. For this reason, she said, public health efforts need to be more locally driven.
“Sometimes what’s decided on a systemic level as a priority really isn’t what the legitimate priority is on the local level by the people most affected. That’s where our voices must be heard,” she said.
‘This is the moment we were waiting for’
Kate Bourne, a member of the St. George COVID-19 task force in Knox County, read early reports of the growing pandemic with dread: “For people in public health, this is the moment we were waiting for.”
Bourne, 62, spent decades with a number of international non-governmental organizations working on reproductive health, HIV and vaccines. Now an independent consultant, Bourne said infectious disease specialists knew the next pandemic was inevitable, it just was a matter of when.
“This is the central worry of our lives — exactly this kind of thing — so the idea of sitting back and not doing anything is anathema to public health people,” Bourne said. “But also Maine communities look after their own and are self-reliant in a lot of ways.”
Margot Kelley, also a member of the St. George task force, said she expected the town select board to lead the pandemic response. “When that didn’t happen, it seemed much too important to just say, ‘OK then.’ ”
Kelley, a retired photography professor, said her experience on the task force taught her effective communication uses clear, succinct and honest messages. “No sugarcoating.”
“That has stood us in good stead because even when the information wasn’t what they wanted to hear, they could trust the sources,” Kelley said.
As a result of the clear messaging, according to Kelley, the local community adhered to safety measures, which allowed schools to be in-person five days a week for most of the year. Most schools in the state have followed a hybrid model of in-person and remote learning throughout this school year.
Boulos, with the Maine Public Health Association, said she’d like to see the task forces morph into local boards of health after the pandemic to address ongoing health challenges and prepare for future ones. Maine statute allows for each town to have a board, she said, but they’re not widespread.
Shah, with Maine CDC, said these groups could continue their “representation and navigation” work with a new disease or different health concern.
“Let’s not forget that even though there is a pandemic of an infectious disease raging, there are other concerns in public health,” he said.
Bourne said she hopes the lesson learned from COVID-19 is that society needs to invest in public health institutions and plan ahead for disasters. And that groundwork needs to include measures to protect the most vulnerable.
“I think (the pandemic) has a bigger lesson for us as a society,” Bourne said. “When we need to build resilience as a community or as a country or as people, we can’t just build resilience for that last thing that happened. Resilience by definition has to be ready to face whatever is coming.”







