When Dr. Christian Inegbenijie agreed to interview for a job as an obstetrician at Down East Community Hospital in the far eastern town of Machias, he barely knew where Maine was. Born in Nigeria and trained in New York, the young physician thought he’d stay for a few years, get some experience in rural medicine, then return to New Jersey or New York for the rest of his career.
Sixteen years later, Inegbenijie finds himself the sole obstetrician delivering babies in a county roughly twice the size of Rhode Island, fighting to save its last maternity unit, one of only 21 left in the state.
Facing a projected decrease in births and spending millions using traveling providers, hospital executives mulled closing the unit. Financially it would have been a logical choice, one that at least nine other Maine hospitals made in the past 15 years, including Northern Maine Medical Center, which closed its obstetrics unit last month.
Fewer than half of the nation’s rural hospitals still offer labor and delivery services, with more than 100 having closed since 2014, according to the Government Accountability Office.
“It’s scary,” said Inegbenijie. “If we would close … I don’t know how that is going to work. Labor and delivery is having a crisis.”
The closure of rural maternity units is dangerous for both babies and mothers, in a country that is already the deadliest in the developed world for women giving birth. Research on the topic in Maine is scant, but national studies show that infant deaths double in counties that lose OB services.

A lack of care after giving birth is also dangerous. New research shows the deadliest time for new mothers is the year after a baby is born, meaning access to postpartum care is critical.
The further from that care a person is, the more likely they are to forgo it, especially in the haze of new parenthood.
And people in rural areas tend to be poorer than urban counterparts, less able to miss work to drive two hours to an appointment.
Inegbenijie is unequivocal about the consequences of closing the last remaining labor and delivery unit in Washington County.
“We would have babies die; we would have moms die. I just have to be blunt.”
A “simmering crisis”
The situation in Washington County is not unique. Eleven of Maine’s 16 counties have just a single hospital offering birthing services. That means those who don’t live nearby one of the remaining birthing hospitals may be forced to travel for hours — often on back roads during poor weather — for care.
The latest obstetrics unit closing came last month, when Northern Maine Medical Center in Fort Kent abruptly announced plans to stop offering birthing services. Hospital officials cited a low number of births and difficulties in hiring nurses. They announced on May 9 they would close the unit less than three weeks later, on the 26th.
In some areas of the state, an hour-long prenatal appointment might now require two hours of driving each way, meaning the loss of an entire day of work, as often as once a week in the later months of a pregnancy. Rural residents carrying high-risk pregnancies may have to go farther — to Bangor, Portland or in rare cases Boston — for a specialist’s care or delivery.
The health of pregnant people in Maine is a “simmering crisis,” wrote Dr. Dora Anne Mills, chief health improvement officer for MaineHealth, in a Facebook post last fall.
The state is the most rural in the nation, with 40% of Mainers living in rural areas — three times higher than the national average — and birth rates that are among the lowest in the country, Mills pointed out. The number of births in the state last year, roughly 12,000, is half what it was in 1960.
“This makes it increasingly difficult for rural hospitals, where the birth rates are even lower, to maintain enough births to keep their labor and delivery units open,” Mills wrote.
But it’s also a self-reinforcing cycle because many experts say places without birthing hospitals have a harder time attracting new families. “The ability of a rural area to offer safe labor and delivery (including c-sections if there are complications) is a pipeline to the future,” Mills wrote.
Women in maternal care “deserts” — areas with no hospitals providing obstetric care, no birth centers, no OB/GYN and no certified nurse midwives — were three times more likely to die during pregnancy or the year after, according to a study of mothers in Louisiana.
Maine, which had the lowest rate of infant deaths in the country in the mid-1990s, now has one of the highest rates in New England, said Kelley Bowden, a retired neonatal intensive care unit nurse and consultant who has helped several Maine hospitals navigate the closure of their maternity units.
And those rates are much higher for certain groups, such as Black and Indigenous Mainers, or those living in poverty; figures that are mirrored nationally. Babies born to people in Maine who have only a high school education are also at higher risk, and are twice as likely to die before reaching their first birthday compared to those born to a parent who has attended at least some college.
The reasons are complicated, but inadequate prenatal care is part of it, said Bowden, who worked on a 2020 report that explored the drivers of infant mortality in the state.
“In the ideal world, everybody’s as healthy as they can be going into a pregnancy, but that’s not what’s happening,” said Bowden. Consistent prenatal care can improve outcomes for babies by managing chronic conditions of people who are pregnant, like obesity and depression.
While Maine does not have any official maternal care deserts, there are still long stretches — 100 miles between Calais and Bangor, 117 miles between Bangor and Houlton — where there is no access to a hospital with a delivery unit.
Meanwhile, relying on an ambulance is becoming increasingly risky because the state’s emergency medical services are facing a crisis of their own. Lifeflight, the air ambulance serving Down East, might take 45 minutes or longer to arrive, said Inegbenijie, in a situation in which minutes matter.
“The burden on (emergency medical services) is another piece to this puzzle,” said Bowden. “If something happens on the way to the hospital, EMS is called and is managing this on the side of the road.”
Maine is also seeing an increase in people planning to give birth at home, usually accompanied by a midwife. Numbers are still low — 323 people gave birth at home in Maine in 2021, up 60% from a decade earlier — just shy of 3% of the total births in the state that year. An additional 40 people gave birth in a “freestanding birth center” in 2021, four times as many as in 2012.
Experts say there could be several reasons for the increase in births outside a hospital — a new licensing system for midwives, implemented in 2020, and an aversion to hospitals during the pandemic — so it’s unclear whether the closure of OB units is affecting the figures or whether the trend will last.
Even if a person plans to birth at home, however, the hospital is always a backup in case something goes awry, which can happen even during low-risk pregnancies. In the past month, Down East had two patients who planned home births show up in the emergency room; both would have died if they had to travel much farther, said Inegbenijie.
“We can’t support it”
The options being weighed by Down East Community Hospital executives this past budget season weren’t good. As staffing costs rose and the number of births slowed, administrators found themselves facing a nearly $1.5 million gap between projected costs and nursing staffing charges in 2023.
There were a few reasons, both helped and hurt by the pandemic. A number of staff, including several in the labor and delivery unit, quit or were let go during COVID for refusing to get vaccinated. Emergency services, which are also crucial in obstetrics in rural areas, faced a similar issue, resulting in long delays transferring patients and increased wait times in the hospital’s emergency department.
To replace the lost staff, the hospital turned to traveling nurses, doctors and techs, paying agencies between $180 and $300 per hour per provider. It also covered the cost of housing, which got increasingly hard to find as buyers snapped up properties during the pandemic.
There was a mini baby boom during COVID, with 190 births at Down East Community Hospital in 2021. But that dropped to 145 last year and is projected to fall even further, to fewer than 100, in 2023. The dip, said John Marshall, the Chief Nursing Officer, is in part due to normal fluctuations and in part to the departure of a popular nurse midwife, who now offers home birth services in the area.
Sixty percent of Down East’s patients are covered by MaineCare, which pays $4,606, on average, for an uncomplicated delivery — not enough, say executives, to cover the costs of the expensive equipment, and highly trained obstetricians, nurses and anesthesiologists who must be on call at all times, and far less than the $14,629 average paid hospitals by private insurers.
The numbers, said Marshall, were clear. “We can’t support it. We just can’t do it.”
Other hospital executives agreed: Delivering babies, at least in a rural area, doesn’t pay. But cutting labor and delivery services, as officials at Mount Desert Island Hospital in Bar Harbor discussed a decade ago, also isn’t necessarily a financially sound decision in the long run. It can make it more difficult to attract doctors to work in other specialties, particularly family practice, who are looking to treat a wide variety of patients, said Chrissi Maguire, the Mount Desert Island Hospital president.
Marshall, who lives in the Washington County town of Princeton, has six children. His wife is a member of the Passamaquoddy tribe, from Indian Township, a population he said relies on the OB services Down East Community Hospital provides. (Rates of infant mortality among indigenous groups in Maine are three times higher than the population as a whole, a figure similar to elsewhere in the country.)
It made Marshall heartsick to think of expecting families being forced to travel for hours to appointments, or delivering babies in the back of an ambulance or the side of the road, unable to get to Eastern Maine Medical Center in Bangor in time.
“We live here in this community, too,” he said. “It’s about serving the community.”
Maguire, of Mount Desert Island Hospital, which is also an independent nonprofit and not part of a larger network, felt the same, adding that the impacts of shutting down labor and delivery services tend to spiral beyond healthcare, making it harder to attract new families to the area. “The greater good of your community is dependent on (it).”
The plan
The strategy devised by Down East Community Hospital executives wasn’t flashy but it was practical: Cross-train nurses from the medical/surgical department, who typically care for patients recovering from or preparing for surgery, in obstetrics. It would require buy-in from staff, said Marshall, and additional work for everyone. But it might, just might, be a way to keep delivering babies.
Stacey Dorr has worked at Down East Community Hospital her entire nursing career, nearly four decades, much of it in labor and delivery. She was there in 2017 when Calais Regional Hospital closed its obstetrics unit, leaving Down East the lone hospital-based OB provider in Washington County. And now she is one of the nurses helping to train others under the new system. The idea that the unit could close brought her to tears.
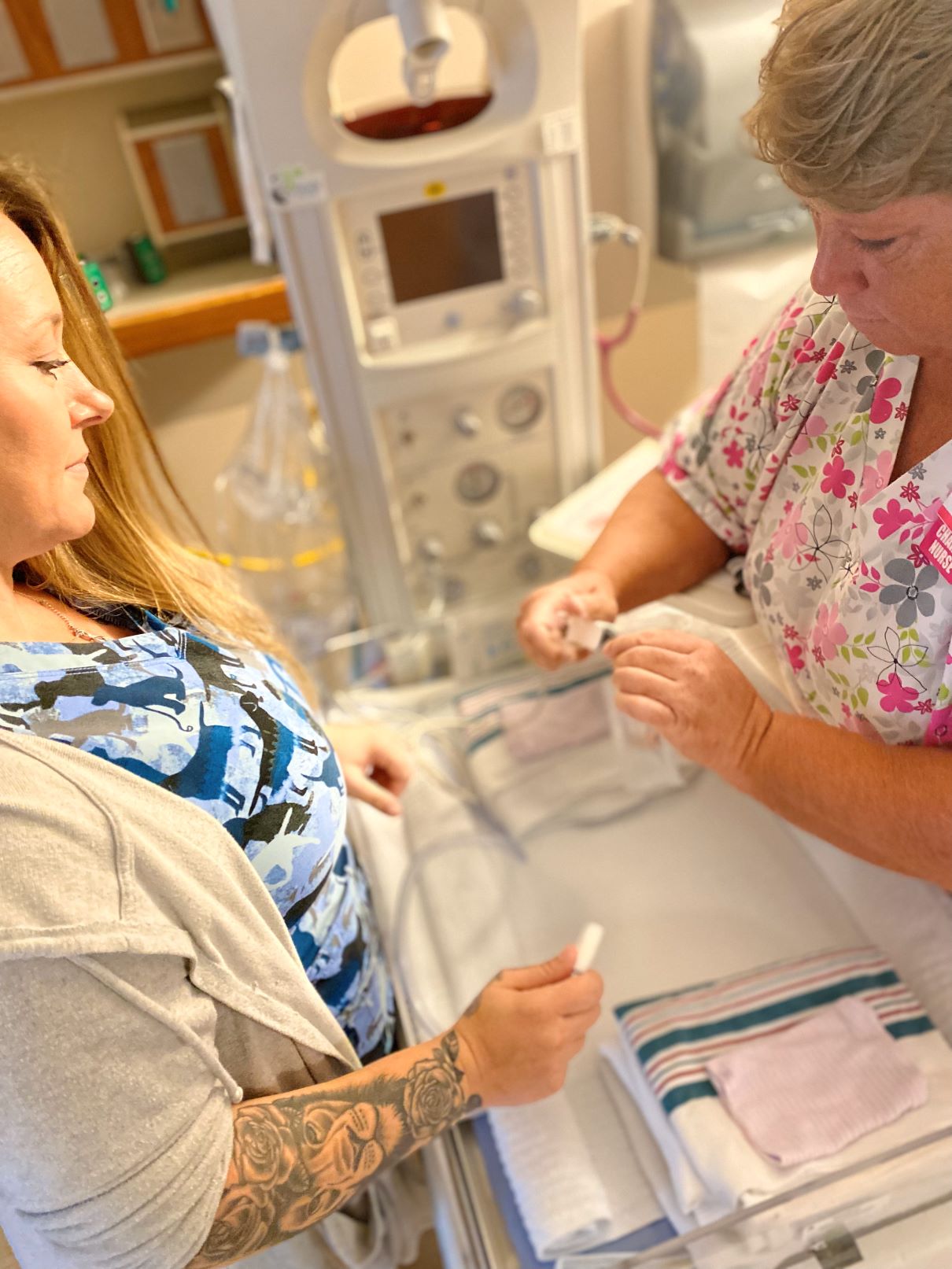
“Having a baby is very personal,” said Dorr. “It starts that person’s life in that community … You build kind of a different relationship than being the nurse for a broken leg or a surgery. People remember you and they appreciate you, because it’s their special day for them and their family. I like being part of that.”
Dorr is grateful to the nurses who agreed to take on a new speciality, one they may not ever have seen themselves in, to help save the labor and delivery service. Melanie Bailey, who was born at Down East Community Hospital and gave birth to one of her sons there, is one of those nurses.
The training has involved both online and hands-on learning in caring for the baby and the person who has given birth. Obstetrics is unusual in that providers have not one patient but two (or more).
While some staff were reluctant at first, said Bailey, “everybody’s been pretty open to learning. I want to do everything I can to keep OB open, and I think everybody else does, too.”
Cross-trained nurses will be trained in resuscitating newborns, a biannual certification. Staffing will change slightly, with just a single dedicated OB nurse on shift rather than two, allowing the hospital to reduce its reliance on traveling providers. A labor-trained medical-surgical nurse will fill in gaps, and a multi-disciplinary team, including emergency department staff, anesthesiologists, a pediatrician, a nursing supervisor and a respiratory therapist, will be on call.
“My life began in this hospital,” said Bailey. “I had my first son in this hospital. It’s very personal for me. Are my children going to live here and have children here? I don’t know. But if they decide to, I want that opportunity for them … I want other people to have that.”
Communities blindsided
If a Maine hospital plans to cut back on maternity services, the state asks executives to inform them, requiring 30 days notice for temporary closures and 120 for permanent terminations.
But those guidelines aren’t always followed. Northern Maine Medical Center announced May 9 that it would shutter labor and delivery services two weeks later, citing declining birth rates and trouble recruiting staff. A spokesperson for the Department of Health and Human Services said the state was notified on May 12 that the hospital would close the unit permanently.
In order to have followed the 120-day guideline for permanent closures, the hospital would have had to notify the state in January.
Even with the required notice, communities are often blindsided. The notice of the closure of the OB unit in Fort Kent caused an uproar among patients and residents, some of whom formed a group, “Save NMMC,” to ensure that the nonprofit “maintains a hospital that adequately serves the people of the region as intended by its founders,” according to a Facebook page.
Bowden thinks hospitals, which plan their budgets at least a year in advance, should be able to strike a better balance between providing more notice to the community and not alienating staff, who may depart en masse once they hear a closure is imminent. (A bill that would have increased notification requirements died in committee this spring.)
Bowden said hospital executives might assume that patients will simply seek the next-closest option. “But that isn’t always accurate. People have strong feelings about local hospitals,” said Bowden. Transportation may also be an issue.
“When Sanford closed their birthing unit (in 2015), the expectation was that, ‘Oh these women will just go to Southern Maine Medical Center (in Biddeford),’ ” said Bowden. “No, you don’t get it. These women don’t have cars. They walk to the hospital, or they take a taxi, or a friend takes them five minutes up the street. You don’t get it … The fact that the executive teams are discussing closure of the OB unit but they’re not including the community and the OB staff — that’s a huge issue.”
The state has several ongoing initiatives aimed at addressing the maternal care crisis, said Dr. Amy Belisle, chief child health officer for the Department of Health and Human Services, and has received millions in federal grants to improve data collection and telehealth services. Last July, Gov. Janet Mills also expanded MaineCare to cover 12 months postpartum, said Belisle, which “we’re hoping is going to be very beneficial.”
Expanded telehealth can play a role in care, said Inegbenijie, the Machias doctor, particularly for postpartum and prenatal visits, and emergency departments can deliver babies, but nothing can replace the care that obstetricians provide.
“This model (proposed by Down East Community Hospital) is a very good model,” said Inegbenijie. “I pray it works.”







