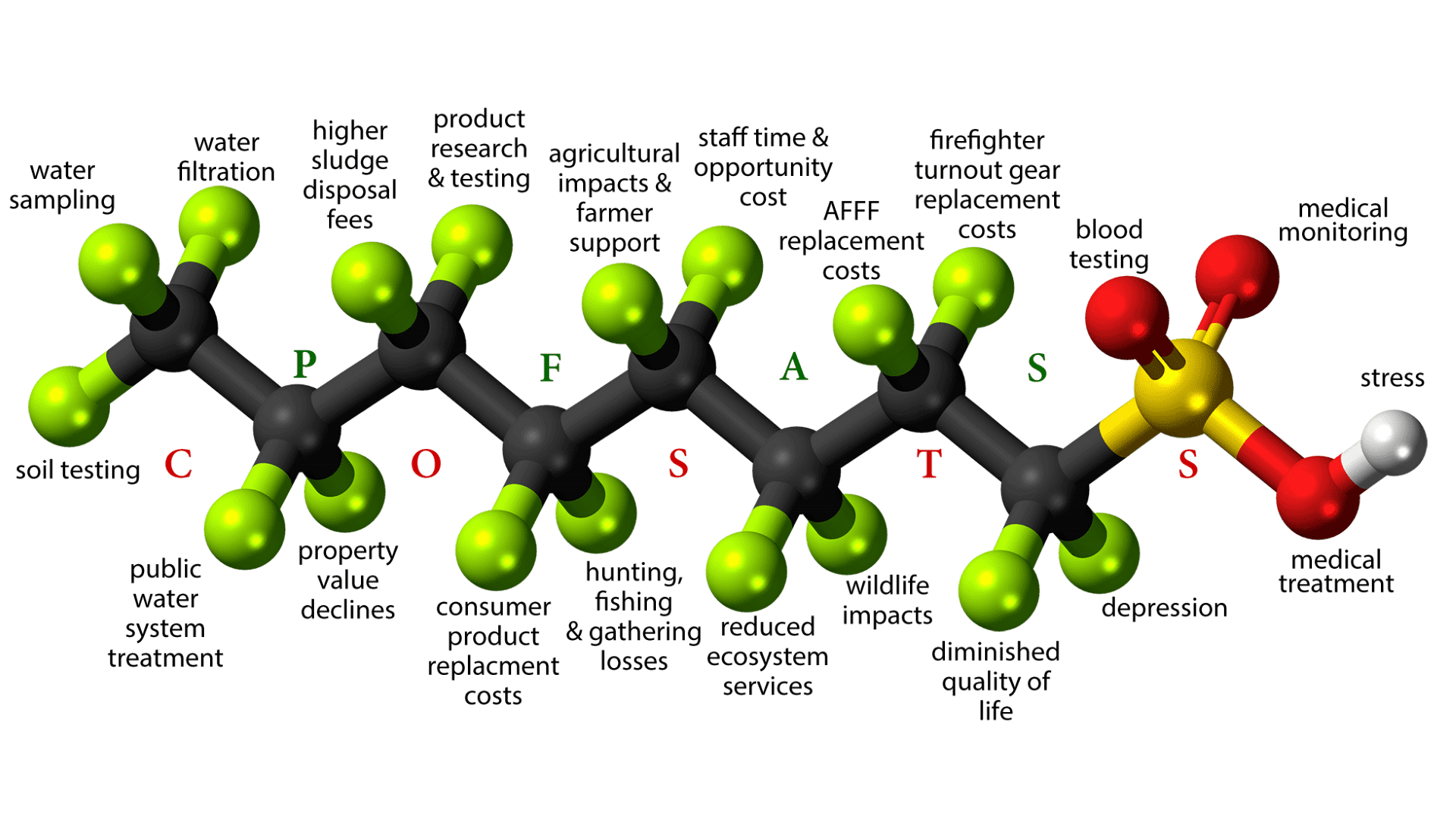
Widespread contamination from per- and polyfluoroalkyl substances (PFAS) “has the potential to impose an unsustainable burden on state and private resources,” the Maine PFAS Task Force wrote three years ago. The weight of that burden from widely dispersed toxic chemicals is now becoming clear in multiplying expenses and costs that defy calculation.
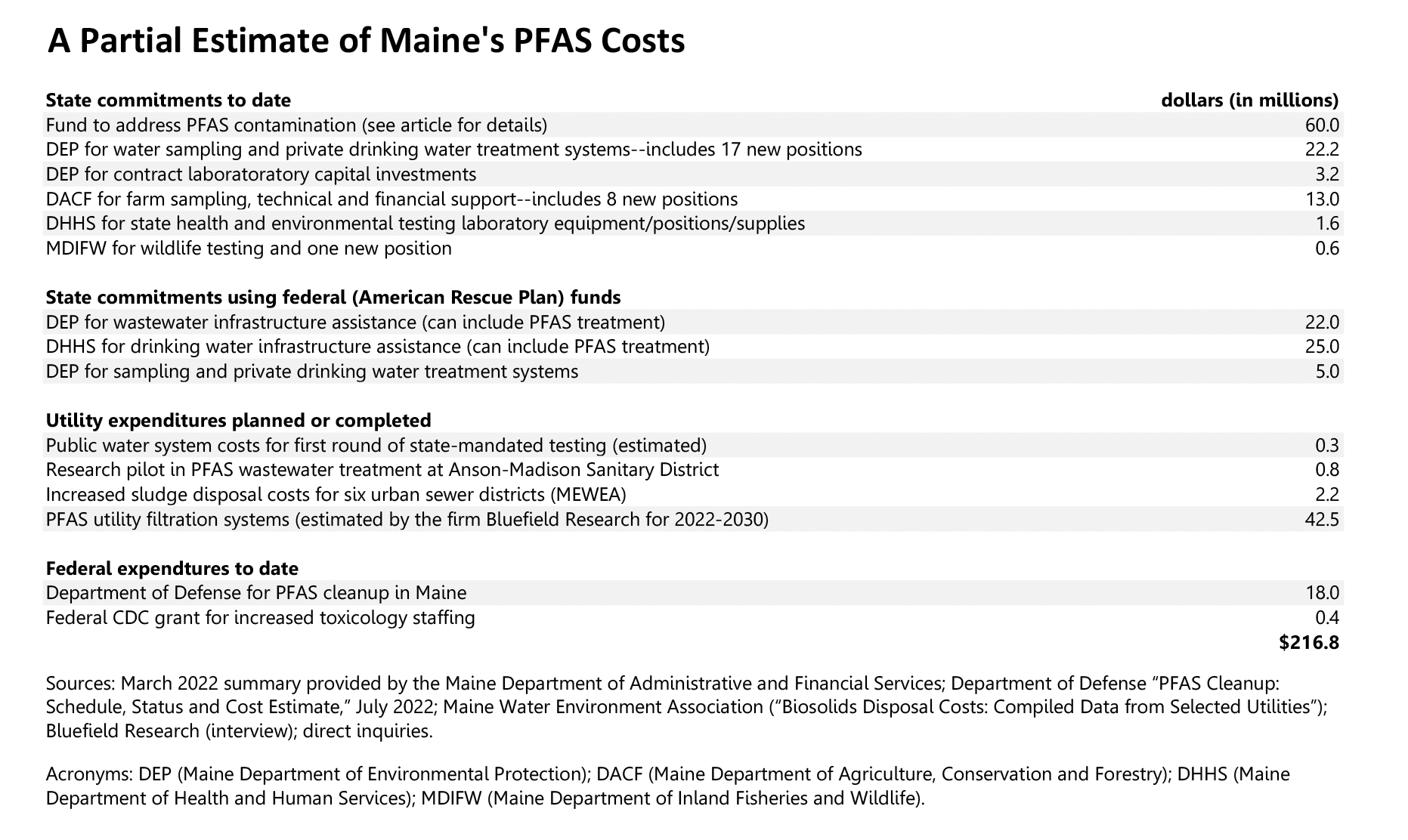
Governmental and utility funds committed to date for early-stage PFAS research and remediation in Maine are estimated to exceed $200 million, according to documents reviewed and inquiries made by The Maine Monitor. Those expenditures represent a small portion of the full economic, ecological and societal impacts (including medical expenses, given the many harmful health effects linked to these industrial chemicals).
Maine has not undertaken a statewide assessment of PFAS costs incurred to date or anticipated. A full accounting across all levels of government and economic sectors could illuminate what long-term impacts PFAS will have on government budgets and taxpayers, and might support legal efforts to recover damages.
RELATED: The long road to recovering PFAS damages
While a few other states have detailed PFAS plans, none appears to have done a comprehensive accounting of related expenses, several experts confirmed. Water treatment costs alone are proving challenging to forecast in settings like Michigan, where by 2020 potential costs totaled nearly $1.5 billion, and Minnesota, which was awarded an $850 million settlement for water remediation in the Twin Cities area that may cost up to $1.2 billion.
Rapidly evolving PFAS research complicates cost-forecasting for water testing, treatment technologies and healthcare. Shifting state and federal regulations generate unanticipated expenses in drinking water sampling and filtration, product testing, and treatment of wastewater and landfill leachate.
An $800,000 research pilot program aimed at getting wastewater at the Anson-Madison Sanitary District to meet the state’s drinking water standard faced additional design challenges when that standard shifted markedly lower. “We are still committed and confident in developing a system” to meet the new standard, district superintendent Dale Clark noted, adding that it’s too early to say whether the $8.5 million in grants and $1.5 million in loans raised to date will cover the full-scale system.
Cost estimates for removing PFAS from leachate at Maine’s two state-owned landfills are not due to the Legislature until January, but a consulting study at Vermont’s only operating landfill, owned by Casella Waste Systems, Inc., estimated PFAS treatment costs over 20 years in the range of $32 million to $394 million.
Unforeseen and unpredictable costs
A new law that requires community water systems, schools and day care centers to report PFAS water-testing results to the state has prompted expenditures for follow-up testing and filtration at numerous sites. Many of those costs have been reimbursed by the Maine Drinking Water Program.
Costs to install smaller filtration systems often run less than $40,000, but there are notable exceptions. Following high PFAS levels in well water, the Houlton Mobile Home Park is working to establish a public water connection reported to cost more than $4 million.
Several larger water districts anticipate PFAS treatment costs on the order of $5-10 million, with research still underway. “Forecasting pricing now is impossible, not difficult,” said Brian Tarbuck, general manager of the Greater Augusta Utility District, given that treatment methods are rapidly evolving and demand for filtration systems is skyrocketing, driving up costs and causing delays on top of existing supply-chain challenges.
Nor can districts budget for the operations and maintenance of the new systems, Tarbuck added, given uncertainty about how long filters will perform and what their disposal costs may be. (Research is underway at the University of Maine on means to destroy PFAS in used filters, but in the short term most filters will go to landfills, contributing to PFAS contamination concerns and costs for leachate treatment there.)
Systems that find PFAS during sampling must test water more frequently, an ongoing expense that drives up operating costs. One district anticipates spending $36,000 annually just on routine water testing for PFAS.
“For the state of Maine, Bluefield (a Boston-based market research firm) forecasts $42.5 million in PFAS drinking water remediation to be spent over the 2022-2030 forecast period,” noted Lauren Balsamo, an analyst at the company, reflecting the fact that Maine is “one of the most pro-active states in terms of testing and implementing regulatory policies. By getting out ahead of impending federal PFAS regulations, states like Maine can avoid fines and penalties later on, which can lead to overall cost savings.”
Through the Infrastructure Investments and Jobs Act, Maine is receiving $7.5 million that can be used for PFAS treatment of drinking water in the first year of a $4 billion multi-year commitment to assist communities with chemical contamination. A quarter of that federal commitment is dedicated to help small and disadvantaged communities, which could help Maine’s smaller public water systems.
Water sampling done to date has found PFAS in some settings with no known sources. The persistent toxic chemicals can travel through groundwater at least a mile or two so it’s unclear how many water sources may have elevated PFAS.
That’s a major concern in a state with roughly 300,000 private wells statewide. About half of Maine households drink water from private wells, which do not qualify for the Infrastructure Act dollars targeted to help small and disadvantaged communities respond to threats like PFAS. Only public-water systems are eligible for those federal funds, according to Jackie Farwell, communications director for the Department of Health and Human Services.
PFAS well water testing and treatment — for those who can afford it
Because it formerly promoted sludge spreading, the state is spending substantial resources over four years testing wells near historically licensed sludge or septage sites. As of Nov. 14, the state had tested 1,185 wells, primarily in locations deemed to be at the highest risk. Among those, 27 percent exceeded the state’s interim drinking water standard of 20 parts per trillion (ppt) for the sum of the six PFAS compounds.
Set to be finalized by June 2024, the state standard may drop. Last June the U.S. Environmental Protection Agency set a lifetime health advisory level near zero for two PFAS compounds, and later this month the agency is expected to propose a national drinking water standard for those compounds.
Given the state’s tiered system for testing sites and its capacity limitations, even people living near sludge-spreading sites have been told they’re not eligible for free PFAS water testing, said Dana Colihan, a co-founder of the community action nonprofit Slingshot. Well owners concerned about other potential PFAS contamination sources, such as military sites, fire stations and training sites, textile manufacturers, tanneries, airports, and settings that may have relied on pesticides or sludge-based compost, are left largely on their own to assess and potentially remediate drinking water.
State-accredited water tests for PFAS typically cost $400 or more. If elevated levels are found, a state tip sheet advises residents to buy and drink bottled water, which can cost $700 or more annually (and bottling companies are not yet mandated to test for PFAS). If well owners decide they need a whole-house filtration system, costs can reach $5,000 (or more if a shed is needed to house the filtration system, such as with manufactured homes).
The high expenses involved in PFAS testing and treatment create “an equity issue in access to clean drinking water,” said Sarah Woodbury, director of advocacy for the nonprofit Defend Our Health. “If you want a test, you should be able to get one. Clean water is a right, not a privilege.”
The state should “look at the barriers to access” for well owners, Woodbury said, including the high financial costs and a testing process that is far from user-friendly, involving price inquiries to multiple labs and research reliant on broadband access. Information on PFAS and testing should be distributed through libraries and medical offices, she added, since some Maine residents, including doctors, are still unaware of the health threats PFAS pose.
A University of Maine survey completed last spring of 432 residents statewide, part of research to be published in Maine Policy Review, found that nearly one in five respondents still had not heard of PFAS. Given the number of Mainers who “have no idea they should get their wells tested,” Colihan said, the state needs to do extensive outreach and consider how to assist low-income and environmental justice communities. While states like New Hampshire have established a rebate system, a direct-pay approach might be better, she said, knowing “some people can’t pay out of pocket even if money is available down the line.”
A case study in the high costs of PFAS
Equity concerns also surface in firefighting. First responders have unwittingly been steeped in PFAS, with the chemicals used in aqueous film-forming foam (AFFF) and protective (turnout) gear, and often present in the smoke from structure fires. Medical costs attributable to PFAS exposure among Maine firefighters are unknown, but the costs of eliminating PFAS from firefighting are becoming clear.
In March, the Maine Department of Environmental Protection offered a rough estimate for a state AFFF takeback program of $2.5 million for collection and disposal, with further resources required for non-fluorinated replacement foam.
Cleanup of Maine military sites that used AFFF has already cost the Department of Defense roughly $18 million, and new expenses keep emerging, such as a PFAS plume from the former Brunswick Naval Air Station that contaminated a well field of the local water district.
AFFF was also used at municipal fire-training areas, potentially reaching nearby wells. The cost to assess such sites for contamination, according to one fire department undertaking this work, can be $50,000, a significant expense for smaller municipalities. If even a third of Maine’s 433 departments needs to undertake such site investigations, the collective costs could top $7 million, not counting funds needed to treat contaminated drinking water sources.
Maine has largely banned AFFF use, but firefighters face ongoing PFAS exposure in multiple layers of their turnout gear, which can cost about $6,000 per set. With an estimated 10,000 firefighters in the state, according to the Maine State Federation of Firefighters, replacement PFAS-free gear could exceed $60 million, not counting disposal costs for the old gear.
According to a report issued in July from the National Academy of Sciences, Engineering and Medicine, firefighters should test their blood for PFAS due to their high occupational exposure. Maine state toxicologist Andrew Smith recently noted that a new blood test covering a broader range of PFAS will soon be available for $490 (not counting the cost of a blood draw, which could increase the total to $600 or more).
Insurance providers in Maine are not required to cover PFAS blood tests and, even when they do, high deductibles can put the cost out of reach for many people. Funding to make the tests accessible to Maine’s current firefighters, not including the unknown number who have retired, could run over $6 million.
Total expenses for firefighting-related PFAS remediation could exceed $75 million without factoring in further water treatment from AFFF contamination or federal defense expenditures. Earlier this month, Congress passed the Protecting Firefighters from Adverse Substances (PFAS) Act, which will help support training guidance, but absent further federal or state help, the costs for replacing firefighting foam and turnout gear, and for investigating fire-training areas, could fall on Maine municipalities.
Costs to agriculture and more
Maine farmers have been at the forefront of responding to PFAS contamination, due to historic spreading of wastewater and industrial sludge onto agricultural fields. The Legislature and Gov. Janet Mills approved a $60 million PFAS Fund this year to support farm families affected by PFAS, potentially providing medical monitoring and medical care, short-term income replacement, support in reconfiguring farm operations to safely produce food where possible, and property buyouts where needed. Additional uses of the fund, outlined in Chapter 10-D of LD 1995, include evaluating the state’s capacity for PFAS testing and data management, conducting related agricultural research, and long-term monitoring of PFAS-contaminated sites. The PFAS Fund Advisory Committee met Dec. 12 for the second time.
To assist farmers before they can access state support, Maine Farmland Trust and the Maine Organic Farmers and Gardeners Association jointly administer a PFAS Emergency Relief Fund to help cover the costs of testing and infrastructure adaptations, as well as income replacement and wellness services. As of Oct. 1, roughly $1.5 million had been raised for the fund and approximately $641,000 had been distributed in grants.
There are still entire sectors where the economic impacts of PFAS have received little study, such as hunting, fishing and tourism, real estate values and insurance. Consumption advisories, for example, can reduce income in rural communities and have disproportionate impacts on families reliant on subsistence hunting and fishing.
PFAS-contaminated properties are likely to lose value, but research as to impacts is only beginning. A Michigan study assessing property value impacts of dioxin, another persistent toxic chemical, found a small but significant reduction in value that remained even if the site was remediated.
Businesses may start to experience financial effects from changing insurance practices concerning PFAS. In recent years, according to the Maine Bureau of Insurance’s Property and Casualty Division, exclusions for coverage of PFAS within commercial lines have become more common.
Costs that resist quantification
Beyond expenses that can theoretically be estimated, there are so many aspects of PFAS contamination that “we don’t know how to quantify or even begin to fully quantify,” observed Alissa Cordner, an environmental sociologist at Whitman College in Washington state and co-author of a 2021 scientific commentary entitled “The True Cost of PFAS and the Benefits of Acting Now.”
Inspired by a European report on the societal, environmental and health impacts from PFAS exposure, Cordner and her colleagues are working to assemble a more complete picture in the U.S. of the “larger costs externalized onto the public” by chemical manufacturers. One longtime PFAS manufacturer, 3M, stated in 2021 that it had paid out “more than $1.2 billion” to treat PFAS pollution. That year, 3M’s annual sales were $35.4 billion, up nearly 10 percent over the previous year.
The highest cost that manufacturers have passed on to the public, the researchers concluded, is the expanding number of human health effects. Virtually every American has PFAS in their blood serum and toxicological research now suggests that for some compounds, virtually no exposure is safe. “In a more equitable world,” Cordner and her colleagues wrote, “this research would be carried out by the producer before the chemical came onto the market.”
A recent study published in the journal Exposure and Health estimated that increased medical bills and decreased worker productivity from 13 medical conditions associated with just two PFAS compounds might cost the U.S. between $5.52 billion and $62.6 billion. “Based on our estimates, the cost of eradicating contamination and replacing this class of chemical with safer alternatives is ultimately justified when considering the tremendous economic and medical risks of allowing them to persist in the environment,” report author and pediatrician Leonardo Trasande wrote.
Even rain now contains PFAS at levels that could prove problematic, not only for human health but for ecosystems. Preliminary scientific research is finding PFAS in virtually all wildlife species tested. While work has been done in recent decades to quantify the economic value of the “services” that ecosystems provide, like purifying water and absorbing carbon, the diminishment of that value due to widespread PFAS contamination has yet to be tabulated.
In undermining the health of Maine’s ecosystems, PFAS have done incalculable damage to cultural and spiritual practices. Toxic contamination from industrial chemicals reduces hunting, fishing and gathering opportunities, and undermines the traditions of Maine’s indigenous tribes, causing generational harm.
For many residents in Maine and beyond, the insidious presence of PFAS has diminished quality of life, and increased stress, anxiety and depression. It’s hard to assign numbers, Cordner noted, to the impact on a parent “knowing that your kid has been drinking contaminated water or the loss felt by a farmer forced to put down livestock.”
Citizens, legislators, agency staff, university faculty, Cooperative Extension staff, advocates and others have expended immense effort to address PFAS contamination, dedicating untold hours that might have gone to other pressing challenges the state faces. No one appears to be tallying that expanding opportunity cost.
“Maine is taking the responsible route, trying to find money to fix what it can,” said Sharon Treat, a former Maine legislator and policy consultant. While the state has filled roughly 30 new positions to contend with PFAS impacts, she said, few if any staff members have been added for essential roles regulating PFAS in products, packaging and pesticides. To prevent future contamination and exposure, she noted, the state needs to invest more resources there.
Maine is paying the price for a “broken national system that continues to allow these untested chemicals to be put in the marketplace,” Treat added. “It’s dramatically more expensive from a financial and health and environmental perspective than if these substances had been caught on the front end.”
This project was produced with support from the Doris O’Donnell Innovations in Investigative Journalism Fellowship, awarded by the Center for Media Innovation at Point Park University in Pittsburgh, Pa.